- Artificial Intelligence (AI)
- Occupational exposure limit values
- Climate Change and Occupational Safety
- List of CMR substances
- Electromagnetic fields
- Endocrine disruptors
- Ergonomics
- Industrial Security
- Collaborative robots
- Noise
- Nanoparticles at the workplace
- Optical Radiation
- REACH
- Reference materials
- Proficiency testing
- Vibration
- Virtual reality
- Work 4.0
Health hazard
Source: Jürgen Fälchle - stock.adobe.com
Hormones regulate important body functions such as development, reproduction and metabolism, and also blood pressure and sleep-wake cycles. They act as messenger substances and are released into the blood by endocrine glands (endocrine: internal) in the body. These glands include the hypothalamus, pituitary gland (hypophysis) and pineal gland in the human brain. Other hormone glands are the thyroid gland (including the parathyroid gland), the adrenal glands, the pancreas and the gonads (ovaries, testicles). The hormones are generally transported to their target tissue through the bloodstream. At their destination, they bind to specific receptors and trigger certain reactions by signal transmission mechanisms, which may be complex. Together with the tissues that produce and receive them, hormones form the endocrine system.

The human endocrine system
Source: Stephan Spitzer
1. What are endocrine disruptors?
According to the definition formulated by the World Health Organization (WHO), on which the definition of the new CLP hazard classes is also based, an endocrine disruptor (ED) is
- an exogenous substance or mixture
- that alters function(s) of the endocrine system and
- consequently causes adverse health effects in an intact organism, or its progeny, or (sub)populations.
The term "endocrine disrupter" thus refers to exogenous chemical substances or mixtures that disrupt the endocrine system of humans and other organisms, thereby causing harm. Substances that influence the hormone system but do not disrupt it so lastingly that a harmful effect occurs are not included in this definition. Substances whose endocrine effect is desirable also lie outside the definition of EDs. The decisive factor for a substance or mixture to be classified as an ED is therefore an irreparable harmful effect; the endocrine effect alone is not sufficient.
Unlike substances that are classified under the CLP Regulation as carcinogenic or sensitising, for example, EDs are not characterised by a more or less clearly defined pattern of harm, but by their toxicological mechanism of action.
This definition alone does not take the potency of substances into account. It does not refer to a dose, nor does it consider the severity or possible reversibility of an effect.
2. Potential health and environmental harm caused by endocrine disruptors
Close interrelationships exist between the hormone, nervous and immune systems. Delicate regulatory mechanisms of the body compensate for the disruption of the hormone system caused by diseases, malfunctions and endocrine active substances. When these regulatory mechanisms cease to be sufficient, harmful effects occur. These disruptions, such as a slight increase in temperature, may be barely perceived. However, they can also be potentially carcinogenic and harmful to reproduction or may interfere with development.
Owing to the multitude of physiological processes that are controlled and regulated by hormones, it is not possible to describe the toxicological effect of EDs as a whole in terms of a small number of health effects.
The updated CLP Regulation lists the following as examples of possible human health disorders caused by substances and mixtures with endocrine-disrupting properties:
- Birth defects
- Developmental disorders
- Reproductive disorders
- Neurodevelopmental disorders
- Cancer
- Diabetes
- Obesity
Harmful effects on the immune system are also associated with EDs.
However, these effects are often based on epidemiological studies whose design is complicated by numerous factors. For example, many endocrine active substances are a natural ingredient in food, including semi-luxury foods. These plant hormones include, for example, flavonoids in soya beans and hops, and lignans in strawberries. It is therefore difficult to identify subgroups in the population with differing exposures but lifestyles that are as similar as possible.
As well as human health, the environment can also be harmed by ED exposure. Endocrine chemicals can have the negative impacts on animal populations described in the updated CLP Regulation. Beyond possible irreversible harm to the development of individual organisms, entire populations of wild animals can be endangered by significant shifts in sex ratios caused by harmful endocrine active substances.
3. Mechanisms of action of endocrine disruptors
Hormones exert their effects by binding to specific receptors in certain tissues. Endocrine active substances can thus directly exert effects resembling those of hormones or anti-hormones on human beings and animals by binding to different receptors in the body.
Substances can also indirectly influence the endocrine system in a variety of ways, for example by accelerating or delaying the production and breakdown of the body’s own hormones. They can influence gene expression or hormone transport or interact with other proteins involved in signalling pathways. They can inhibit or activate enzymes that disrupt the uptake and transport of hormones from cells. Epigenetic effects on genes (caused for example by DNA methylation) have also been described for endocrine active substances; these effects are, however, still relatively unclear.
Research in this area is focused on substances that impair reproduction. These include substances with estrogenic and androgenic properties and those that influence the synthesis of steroid hormones. Substances that affect thyroid function are also being studied. This is the origin of the widely used abbreviation EATS (estrogen, androgen, thyroid, steroidogenesis): it refers to the four main ways in which EDs can affect the endocrine system. Most of the OECD tests developed to date for the study of ED properties relate to mechanisms of action concerning EATS.
However, a growing focus is being placed on substances that influence the hypothalamic-pituitary-adrenal (HPA) axis, also known as the stress axis. The HPA axis is the main part of the hormone system controlling responses to stress. In addition, evidence is growing of substances that influence hormones’ control of the metabolism and may be involved in the development of obesity and diabetes. New methods for identifying such substances are needed.
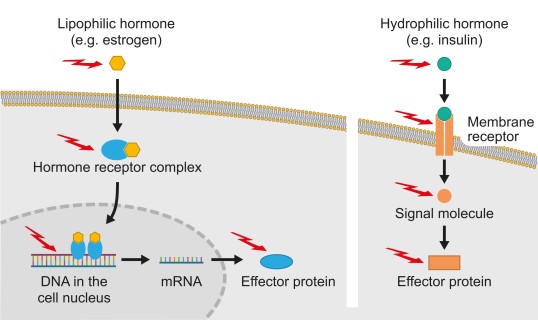
Examples of mechanisms of action: endocrine disruptors can interact with hormone receptors and ligands and influence signalling pathways within cells. Fat-soluble (lipophilic) and water-soluble (hydrophilic) hormones differ in their signalling pathways, which offer many targets for endocrine disruptors. Fat-soluble steroid hormones such as estrogen can penetrate the cell membrane, bind to receptors in the cytoplasm or cell nucleus and trigger the production of proteins (effector proteins) that influence the metabolism. In the case of water-soluble hormones it is the signal, not the hormone itself, that is transmitted into the cell. For example, catecholamines or insulin bind to a receptor on the cell membrane, and the signal is transmitted into the cell. The insulin signal leads to increased production of glucose transporters in muscle cells, causing glucose uptake to rise. (Source: Gottfried, E.: Wie wirken endokrine Disruptoren? Pharmazeutische Zeitung, October 2022)
Source: Stephan Spitzer
4. Examples of endocrine active substances

Source: photka -- stock.adobe.com
While ethinyl estradiol, for example, is used intentionally as a synthetic sex hormone in contraceptive preparations, the disruptive influence of other synthetic substances upon the hormone system is an undesired side-effect. A large number of chemicals are considered to be endocrine. They are found not only in pharmaceuticals and cosmetics, but also in certain pesticides, biocides and preservatives (e.g. butylparaben). Among the best-known synthetic endocrines are intermediates used for plastics, such as bisphenol A, and plasticisers, such as certain phthalates used in plastics manufacturing. Surfactants such as nonylphenol and certain flame retardants from the group of polybrominated diphenyl ethers and polychlorinated biphenyls (PCBs) can also affect the hormone system in a range of ways.
Many natural substances with potentially endocrine properties are also found in our food. Examples are secondary plant compounds such as phytoestrogens in beer hops or broccoli, and isoflavones from the soya bean, which among other effects also have an estrogenic effect. However, this does not necessarily mean that they act as endocrine disruptors; as with all toxic substances, whether they do so depends largely on their dose.
During their production and use, many of these substances enter the environment and thus the main environmental compartments, such as water and soil. From there, they find their way into drinking water and the food chain and can be ingested by any person.
5. Do effect thresholds for endocrine disruptors exist?
The basic principle in toxicology is that the dose is the measure of a substance’s toxic effect. It is therefore often possible to determine a "no observed adverse effect level" (NOAEL), i.e. the highest concentration of a substance that is shown in human or animal studies only just to fail to have any adverse health effects. A certain threshold is assumed to exist below which undesirable effects can be ruled out as being highly unlikely.
However, the buzzwords of "low-dose effects" and "non-monotonic dose-response relationships", which are U-shaped or bell-shaped but may also take other forms, are associated with strongly diverging views of whether a harmful effect of a substance can occur at a lower dose and even at a dose far below an NO(A)EL determined in accordance with established guideline test procedures. Consistent with the endocrinological principle that even very low quantities of hormones are sufficient to interact with a receptor and trigger a corresponding receptor response, some experts assume that endocrine active substances can cause low-dose effects.
Some endocrine disruptors, a chemically very heterogeneous group, do in fact appear to exhibit non-monotonic dose-response relationships. Such a substance property is, however, difficult to prove, as at low doses, it is difficult to distinguish between the effects occurring and the unavoidable background noise produced by the test method. Such a low-dose effect is also generally not limited to endocrine activity. For example, the essential trace element cobalt is a key ingredient of vitamin B12, the reason why cobalt deficiency leads to blood clotting disorders and nerve damage. Conversely, excessive exposure to cobalt can result, among other things, in liver and heart disease, and even malignant tumours in rodents. In relatively low concentrations, cobalt can also cause allergic contact dermatitis.